Chatbots are the key enabler of any eHealth initiative
20 January, 2022
The current pandemic has accelerated digital transformation in all sectors, including health. A huge number of digital health (or e-health) initiatives have proliferated and accelerated in the last couple of years.
Broadly speaking, digital health refers to “tools and services that use information and communication technologies (ICTs) to improve prevention, diagnosis, treatment, monitoring and management of health-related issues and to monitor and manage lifestyle-habits that impact health” (source: EU Public Health).
Any major disruption in the health sector, like the one we are experiencing right now, brings plenty of new opportunities but also many challenges, as our society must learn and adapt to this new reality. In this post, we argue that chatbot technology is key to maximizing the benefits and minimizing the risks associated with this movement towards mass adoption of e-health in both the public and private health sectors.
Chatbots are computer programs that are able to maintain a conversation in a natural language (i.e. English, Spanish, Catalan, etc.) with a user. As such, they can make interfaces more convenient and understandable for all types of user profiles. Thanks to their natural language processing (NLP) capabilities, chatbots are able to ‘understand’ users’ requests and automatically process and/or answer them.
This automation is key to reducing the burden on the health system and health professionals. Bear in mind that digital transformation will not really be able to mitigate the pressure on the (public) health system unless we understand that this transformation must be accompanied by a transformation of who is actually supposed to do the work.
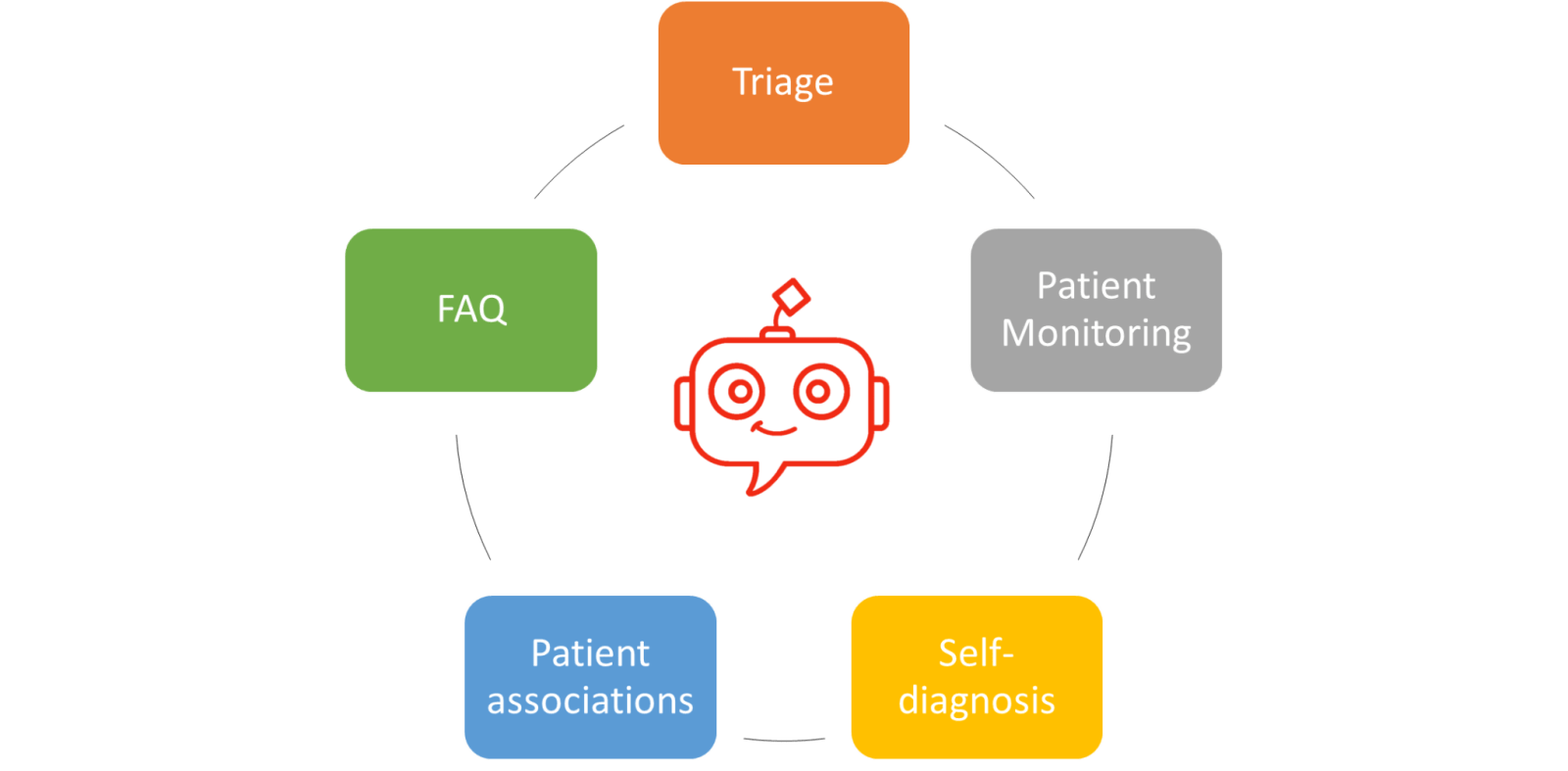
In this sense, chatbots could have a major impact in almost any e-health domain. Let’s look at some of them.
- Patient triage. The COVID pandemic has shown us that we need a quick way to sort patients calling emergency lines, to identify those that request urgent attention from those that were just asking for information. A chatbot (in particular, a voicebot, i.e. a chatbot with speech-to-text and text-to-speech capabilities to process phone calls or other types of voice messages) could be used to optimize the triaging process.
- Patient monitoring. Many health treatments require some type of patient supervision. Chatbots could take care of this monitoring and alert the doctors when there is an unusual answer or data point that calls for their attention.
- Self-diagnosis. Nothing can replace the opinion of a medical expert. But, unfortunately, often people just google their symptoms when trying to understand whether they are suffering from some type of physical or mental condition. This is especially true in some age ranges (e.g. teenagers, for whom bullying can be detected using TrustBot) and for some types of diseases (e.g. sexually transmitted diseases). Bots with expertise in specific diseases could be a better alternative. They would be trained by experts in the disease, and would provide a safer alternative than a Google search. It is worth remembering that not everybody has the privilege to have access to a doctor.
- Patient associations. For rare diseases in particular, these are a very valuable information resource for new patients. As such, the same set of questions is repeatedly asked by people trying to learn about their new condition and what to expect from it. A chatbot could be used to provide this first interaction.
- FAQs. Frequently asked questions are also common in the health domain, and not only in relation to diseases or treatments, as discussed above, but also regarding the many different administrative procedures. As an example, in recent months, health centres have been flooded with questions regarding where to go to get a vaccine, what documentation was needed, how to make appointments, etc. These questions were often directed at health professionals such as family doctors, who had no part in these decisions and were just wasting their time redirecting the questions.
At Xatkit, a spin-off of the SOM research group, we are exploring some of these scenarios together with other partners from XarTec Salut, a network of 47 research groups from 17 different institutions, with the goal of fostering entrepreneurship and innovation in health tech.
The first question we posed ourselves was why, if chatbots are so useful, weren’t we seeing a massive adoption of chatbots in e-health already?
There are two main answers to this question.
- Educational challenges: many people prefer to talk with ‘humans’ and not with ‘machines’. We should emphasize the benefits of chatbots while always combining a chatbot with a live chat solution. With this approach, we can reassure users and clarify that if the chatbot fails or they are not satisfied with the chatbot’s answer, they can always request to talk with a human. New generations are obviously much more familiar with bots and therefore reticence towards this type of technology should diminish in the near future.
- Technological challenges: building a good chatbot is far from easy. Chatbots must combine AI techniques (for the natural language processing part) with software automation techniques, and must deal multi-channel deployment requirements. And their design involves an interdisciplinary team that should adhere to strict open and transparency practices. Moreover, health bots have additional requirements due to their critical impact. Indeed, they should be treated as a safety-critical system to avoid potentially deadly mistakes (e.g. a bot giving the wrong advice to patients or missing the fact that the monitored patient’s status requires immediate medical attention).
Clearly, we still have work to do before chatbots can be deployed en masse across all layers of the health sector. But, this is clearly the future and the only solution that will be effective against this and any future health crisis. At Xatkit, we, along with many others, have started working towards this future. Will you join us?